One more hope to tackle Type 1 Diabetes
Diabetes is an endocrine disease characterized by high blood sugar level due to either deficient insulin production by pancreas or the body cannot use the produced insulin effectively. Almost 463 million people of the world had diabetes as of 2019. Generally, diabetes is categorised into Type 1 and Type 2. Type 1 diabetes is an insulin-dependant diabetes in which a patient is unable to produce sufficient amount of insulin required in the body. In Type 1 diabetes, insulin producing β cells present in the pancreas (pancreatic islets) are destroyed leading to insulin deficiency. The exact cause of Type 1 diabetes is still not clear and the effective preventive measures are also not known. Hence, to address this issue, the researchers from Massachusetts General Hospital have developed a transplantation method of pancreatic islets to cure Type 1 diabetes. In earlier studies, the β cells were transplanted into liver which has several limitations; thus, in this method, the researchers used omentum as the site of transplantation. The experiment was successful in non-human primates, as these animals could maintained with normal blood glucose levels and insulin secretion was restored. Thus, the findings could revolutionize the treatment strategy for Type 1 diabetes and therefore, the investigators are planning for a future human trial.
Sources:
- Bioengineered omental transplant site promotes pancreatic islet allografts survival in non-human primates. Cell Reports Medicine, 2023.
iNCOVACC: Another COVID-19 vaccine from India
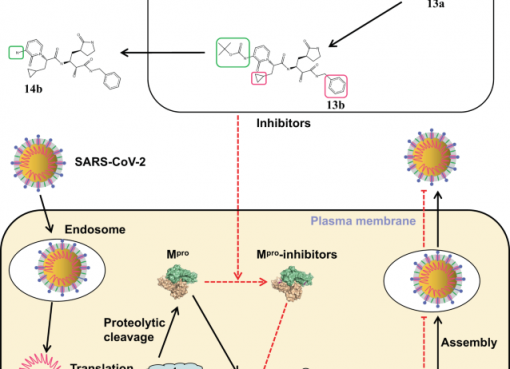
The COVID-19 pandemic is still a nightmare and many sporadic outbreaks are reported from different corners of the globe. Although, several COVID-19 vaccines were developed across the globe, the loopholes and side-effects are getting unrevealed day-by-day. Thus, the race to produce a safe, effective and potent vaccine is still on among the scientific community. In this race, recently the Central Drugs Standard Control Organisation (CDSCO) of India approved a new intranasal COVID-19 vaccine ‘iNCOVACC’ for emergency use in adults who are 18 years or above in age. The vaccine was developed by Bharat Biotech International Limited (BBIL) in collaboration with Washington University in St Louis, US. It is a recombinant adenovirus vectored vaccine that encodes spike protein of SARS-CoV-2; however, it is replication-deficient. The vaccine successfully passed the clinical phases I, II and III. This vaccine candidate can produce strong humoral and long-lasting cell-mediated immune responses. The vaccine was formulated for intranasal delivery as nasal drops which will help in mass vaccination with an easy painless administration. The iNCOVACC is designed for a two-dose schedule at four weeks interval, and a heterologous booster dose. It is stable at 4-8 °C for storage and distribution. The vaccine will be cost-effective for low- and middle-income countries which will be helpful in prevention and control of COVID-19 pandemic or epidemic.
Sources:
Novel antibody to fight deadly snake bites
Bites of venomous snakes can be life-threatening. As per World Health Organization (WHO) report, about 5 million people are bitten by snakes annually. Out of these, almost 2 million are clinically affected and approximately 100000 die due to the bite of poisonous snakes. Antivenoms produced in animal can effectively be used to prevent and reverse the toxicity of snakebite envenoming. However, these antivenoms sometime produce adverse reactions in certain individuals which are severe in nature. Thus, there is always a search for a safe therapy to protect people from severe snakebite envenoming. In this context, scientists from multiple institutes have generated a novel human origin monoclonal antibody by using phage display technology that is capable of neutralizing the venom of Asian elapid and African snakes. The prototype treatment with human monoclonal antibody was found to be effective against certain species of snakes that produce potent neurotoxins such as Cobra, Mamba and Krait.
Sources:
- Discovery and optimization of a broadly-neutralizing human monoclonal antibody against long-chain α-neurotoxins from snakes. Nature Communications,
Another patient totally cured from HIV by Stem cell transplantation therapy
Human immunodeficiency virus (HIV) is the causative agent of Acquired immuno-deficiency syndrome (AIDS). As of 2021, approximately 40 million people are living with HIV infection in the globe. About 1.5 million new cases of AIDS and 0.65 million deaths due to HIV infection are reported annually. There is no effective cure or vaccine against AIDS. However, the scientists from different corners of the world are trying different strategies to cure AIDS. Till date, two HIV patients were cured totally using stem cell therapy and recently a third patient has been cured completely using stem cell transplantation. The third patient received stem cells from a donor who has a special mutation in the HIV-1 co-receptor CCR5. This particular mutation disables HIV to entre CD4+ T-lymphocytes. Thus, the patient did not produce specific antibodies or reactive immune cells against HIV as well as the patient was devoid of replicating virus after the stem cell transplant. The patient was declared to be HIV free after closely monitoring for 14 years post stem cell transplantation. The findings of this study will give valuable insights to develop effective treatment strategy to cure AIDS in future.
Sources:
- In-depth virological and immunological characterization of HIV-1 cure after CCR5Δ32/Δ32 allogeneic hematopoietic stem cell transplantation. Nature Medicine,